Most of us can rattle off our phone number, our kids’ birthdays, maybe even our high school locker combination. But when it comes to the numbers that actually tell the story of our health? A lot of us go blank.
That’s not a criticism — it’s just reality. We’re busy. These things don’t always come up unless a doctor puts them in front of you. But knowing a handful of key numbers can make a real difference in catching problems early, understanding your risk, and feeling more in control of your own wellbeing.
Here are five numbers worth knowing — and what they’re actually telling you.
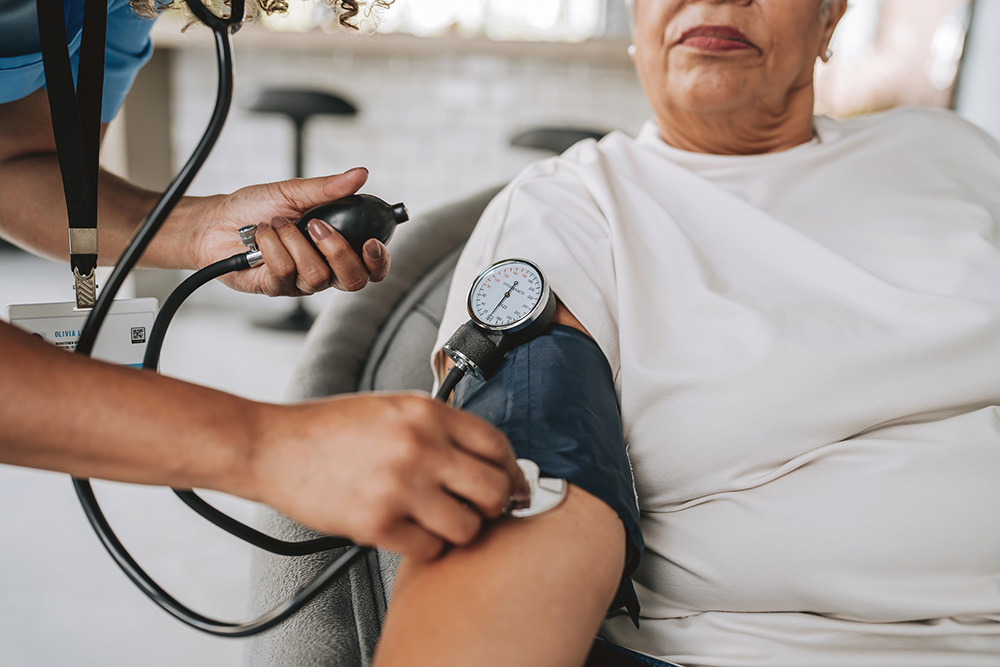
1. Blood Pressure
What to aim for: Less than 120/80 mmHg
Blood pressure is one of those things that earns the nickname “the silent killer” for good reason. High blood pressure often has no symptoms at all — you can feel completely fine while it’s quietly putting stress on your heart, arteries, kidneys, and brain.
The two numbers you see on the cuff represent the pressure in your arteries when your heart beats (systolic, the top number) and when it rests between beats (diastolic, the bottom number). Together, they give your doctor a window into how hard your heart is working.
The good news: blood pressure responds well to lifestyle changes. Movement, a lower-sodium diet, managing stress, and limiting alcohol can all move the needle—sometimes significantly. If lifestyle changes aren’t enough, medication works well and is widely tolerated.
When did you last have yours checked? If it’s been more than a year, it’s probably time to do so.
2. Blood Sugar (Fasting Glucose or A1C)
What to aim for: Fasting glucose under 100 mg/dL / A1C below 5.7%
Type 2 diabetes doesn’t usually announce itself. It tends to develop gradually, often spending years in a “prediabetes” range before tipping over—and by the time symptoms show up, some damage has already been done.
Your fasting blood sugar gives a snapshot of your glucose level at a single point in time. Your A1C, on the other hand, reflects your average blood sugar over the past two to three months, making it a more complete picture.
Why does it matter? Chronically elevated blood sugar affects nearly every system in your body—your eyes, your nerves, your kidneys, your cardiovascular system. Catching it early, when you’re still in the prediabetes range, gives you a real chance to reverse course through diet, exercise, and weight management before medication ever enters the conversation.
3. Cholesterol (Lipid Panel)
What to aim for: Total cholesterol under 200 mg/dL, LDL under 100 mg/dL, HDL above 40 (men) or 50 (women)
Cholesterol gets talked about a lot, but it’s often misunderstood. Cholesterol itself isn’t bad, and in fact, your body needs it. The issue is when certain types build up in your arteries and increase your risk of heart attack and stroke.
Your lipid panel breaks it down into several numbers:
- LDL (“bad” cholesterol): the kind that accumulates in artery walls
- HDL (“good” cholesterol): the kind that helps clear LDL out of your bloodstream
- Triglycerides: fats in your blood, often tied to diet and alcohol intake
Your doctor will look at these numbers in context (alongside your age, family history, blood pressure, and whether you smoke) to get a clearer sense of your overall cardiovascular risk. Numbers alone don’t always tell the full story, which is exactly why this conversation belongs in a doctor’s office, not just on a lab printout.
4. Body Mass Index (BMI)—With Some Important Context
What to aim for: 18.5–24.9 (standard range)
BMI gets a fair amount of criticism, and honestly, some of it is warranted. It’s a simple calculation (weight divided by height squared) and it doesn’t account for muscle mass, bone density, where you carry fat, or a number of other factors that affect health.
That said, it’s still a useful starting point. Consistently elevated BMI is associated with higher risks of heart disease, type 2 diabetes, sleep apnea, joint problems, and certain cancers. It’s a data point, not a verdict.
What matters more than the number on its own is the trend over time and how it fits alongside your other health markers. Someone with a BMI of 27 who has great blood pressure, healthy glucose, and stays active is in a very different situation than someone with the same BMI and several other risk factors piling up.
Your doctor can help you interpret what your BMI actually means for you and what, if anything, it suggests you focus on.
5. Resting Heart Rate
What to aim for: 60–100 beats per minute; lower (within reason) is generally better
Your resting heart rate should be taken when you’re calm and still, ideally first thing in the morning, and is a surprisingly useful window into your cardiovascular fitness and overall health.
A well-conditioned heart pumps blood efficiently, so it doesn’t have to beat as often to do its job. Consistently low resting heart rates (think 50s or 60s) are common in people who exercise regularly. On the flip side, a resting heart rate that’s chronically elevated especially above 80 or 90 can signal that your heart is working harder than it needs to, which is worth talking to your doctor about.
It’s also a number that changes. If you’ve started exercising more, you’ll often see it drop over time. That’s your body adapting, and it’s a genuinely encouraging thing to track.
Putting It All Together
None of these numbers exist in a vacuum. A single data point rarely tells the whole story, and that’s exactly why an annual wellness visit matters. It’s not just about treating what’s wrong. It’s about understanding where you are, spotting trends before they become problems, and building a relationship with a provider who actually knows you.
If you’re not sure where your numbers stand, that’s the right place to start. You should be staying on top of your health with an annual wellness exam or physical, or at least checking in with your primary care provder once a year. If you’re overdue for a visit or checkup, give us a call—we’d love to see you!